|
However, DXA has important limitations in the evaluation of the fracture risk in a growing child. Bone health monitoring, identification of at-risk patients and timely intervention is thus an important part of the management of DMD.ĭual-energy X-ray absorptiometry (DXA) is the standard measure of bone mass and density for clinical use in children. Patients with mild or even asymptomatic fractures may have a high risk of future vertebral fractures. The long-term consequences of permanent deformity on pain and function following repeated childhood vertebral compression remain unstudied. Vertebral fractures may cause severe pain, but may also be asymptomatic and thereby underdiagnosed. įractures in the long-bones are painful and can be detrimental to the ambulatory function of a patient with DMD, especially if they occur in the late-ambulatory phase. Further, steroid induced obesity, poor linear growth, hypogonadism and pubertal delay add to the complexity of bone health evaluation in GC treated DMD. GC treatment is also associated with 25-hydroxy-vitamin D (25(OH)D) deficiency and by itself increased fracture risk. GC treatment exacerbates the situation by disrupting the osteoblast-osteoclast balance and coupling, compromising the biomechanical properties of bone, and inhibiting the absorption of calcium from the gastrointestinal tract and the reabsorption of calcium in the renal tubuli. These findings indicate significant reduction in bone formation and a relatively increased bone resorption (increased endosteal resorption). Moreover, the total trabecular bone volume per total volume was reduced, due to a reduction in trabecular thickness. Thus, the total length of the bone biopsy was reduced, as was the cortical shell (thickness). Histomorphometric analyses of bone biopsies in DMD showed clear differences in all compartments between patients with DMD compared to healthy age-matched reference data. In untreated DMD, it is suggested that reduced bone strength is related to decreased muscle tension on bone and muscle disuse as well as nutritional factors, disturbances in the calcium homeostasis and increased activity of inflammatory cytokines. 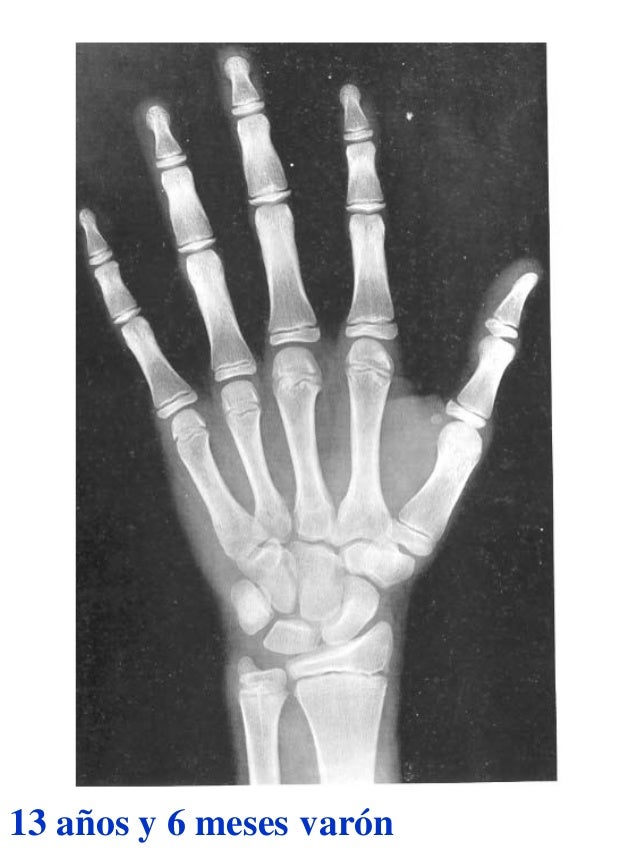
Several studies have described a higher incidence of low-trauma long-bone (appendicular) fractures in steroid-naïve boys with DMD compared to the normal population, and a significantly increased risk of appendicular and vertebral fractures in glucocorticoid (GC) treated DMD. Low Bone Mineral Density (BMD) and an increased risk of fractures is a well-established consequence of many chronic diseases in childhood, including Duchenne muscular dystrophy (DMD). The physiological process of bone modelling and remodelling in childhood involves complex and sensitive endocrine and immunological signalling systems, which may be affected by factors such as physical conditioning, poor linear growth, obesity, pubertal delay, vitamin D deficiency, and alterations in calcium homeostasis. Our results suggest that skeletal maturation should be assessed in the evaluation of short stature and bone health in GC treated boys with DMD, as failing to consider delayed bone age leads to underestimation of BMD Z-scores and potentially overestimation of fracture risk. When BMD Z-scores were corrected for by retarded bone age, the increase in BMD Z-scores was significant for all age groups. Mean BMD Z-scores fell below − 2 before 12 years of age in the glucocorticoid treated group, with scores significantly correlated with age, duration of treatment and pubertal development. The difference in height between glucocorticoid treated and naïve boys was no longer significant when height was corrected for delayed skeletal maturation. Bone age was significantly delayed, and the delay increased with age and duration of treatment. 
The participants in the glucocorticoid treated group were short in stature and puberty was delayed. The relationship between bone age, height and bone mineral density (BMD) Z-scores was explored. MethodsĪs part of the Norwegian Duchenne muscular dystrophy cohort study, we examined the skeletal maturation of 62 boys less than 18 years old, both currently glucocorticoid treated ( n = 44), previously treated ( n = 6) and naïve ( n = 12). Monitoring of endocrine and skeletal health and timely intervention in at-risk patients is important in the management of children with DMD. Low bone mineral density and an increased risk of appendicular and vertebral fractures are well-established consequences of Duchenne muscular dystrophy (DMD) and the risk of fractures is exacerbated by long-term glucocorticoid treatment.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
